Adrenal Gland Calcification
Adrenal calcifications are an unusual finding on computed tomography or plain radiographs of the adrenal glands. Although the underlying causes of adrenal calcifications are numerous, in certain instances, the appearance and pattern of calcifications combined with additional radiographic features and the appropriate clinical context can assist in the elucidation of the possible differential diagnoses.
Pathophysiology of adrenal calcification
Calcification (which is the abnormal deposition of calcium salts at extraskeletal sites), has two distinct subtypes. Dystrophic calcifications involve the accumulation of calcium salts in degenerated or dead tissues. There is usually normal calcium homeostasis.
Metastatic calcifications, on the other hand, are typically seen in disorders of calcium homeostasis which results in ectopic deposition of calcium in various tissues.
Areas of dystrophic calcification in adrenal tissue occur in the setting of necrosis of any type. For example, caseous necrosis (tuberculosis), liquefaction necrosis (chronic abscesses), dead parasites (hydatid cyst), and hematomas are associated with dystrophic calcification.
Significance of adrenal calcification
It is worth noting the morphology and pattern of adrenal calcification, attenuation of the adrenal gland (non-contrast computed tomography) and focality can assist in making the right diagnosis. Even more importantly, needless biopsies and incorrect management decisions can be averted if a clinicopathophysiologic approach is used in the evaluation of adrenal gland calcifications.
Etiology of adrenal calcification
| Etiology | Calcification morphology | Clinical features |
| Myelolipoma | Adrenal myelolipomas are composed of primarily fat (CT attenuation value). Rarely can become secondarily calcified (saponification) with only small areas of fat | A nonfunctioning, nonmalignant neoplasm which is composed of fat and hematopoietic tissue and on rare occasions areas of calcifications |
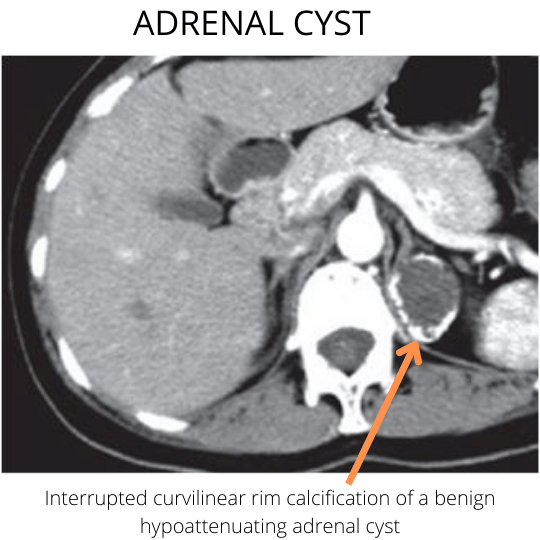
| Adrenal hemorrhage | Hemorrhage over time is reabsorbed, leaving behind a non-enhancing pseudocyst with a rim of peripheral calcification. | An acute adrenal hemorrhage presents as an adrenal mass with a very high attenuation value (upwards of 50 Hounsfield units) |
| Adrenal Abscess | An chronic arsenal abscess can present with a non-enhancing cystic lesion with a rim of peripheral calcifications. | May be due to primary seeding by an infectious agent due to sepsis or secondary infection of an adrenal hematoma |
| Adrenocortical carcinoma (ACC) | Highly variable and nonspecific pattern of calcification. Gross invasion of an adrenal lesion into the adrenal veins or renal vein is pathognomonic for ACC. | |
| Adrenal metastases | A high attenuation value on non-contrast tomography differentiates a benign from a possible malignant adrenal process. Tumors associated with adrenal calcifications include papillary thyroid carcinoma, osteosarcoma, and mucinous adenocarcinoma. | |
| Adrenal adenomas | Calcification in adenomas is unusual. Hemorrhagic conversion and secondary fibrosis may present with large, heterogeneous internal calcifications. | |
| Pheochromocytoma | Pattern of nonspecific calcification | |
| Granulomatous conditions. | A thick and irregular pattern of calcification. The adrenals may become atrophic and significantly calcified in cases of chronic granulomatous diseases. | Occur in chronic granulomatous diseases like histoplasmosis and tuberculosis |
| Hemangioma | They classically contain phleboliths (areas of calcification in vessels) | |
| Teratoma | Like myelolipomas, teratomas contain fluid, fat, and possible calcifications. A fat-fluid level is pathognomonic for an adrenal teratoma. | These are neoplasms that arise from embryonic germ cells that fail to migrate to their designated gonadal position. |
| Neuroblastoma | These tumors undergo necrosis and hemorrhagic transition and may be calcified in up to 85% of patients. | Derived from sympathetic ganglia including the adrenal medulla (a large sympathetic ganglion). Usually seen in the pediatric population. |
| Lipid storage diseases | An accumulation of triglycerides and cholesterol esters in not only the adrenals but other organs as well. | Abdominal enlargement due to hepatosplenomegaly. Seen in pediatric patients. |
| Hydatid cyst of the adrenal gland | Very well-circumscribed multicystic mass of a unilateral adrenal gland. Scattered areas of calcification. |
Radiographic findings of adrenal calcification
This is a simple algorithm to identify the differential diagnoses of adrenal calcifications. Enter the relevant CT findings in the form.
You will need the following parameters: morphology and pattern of calcification. The attenuation value on non-contrast computed tomographic will assist in further characterization of the calcified adrenal lesion.
References (Suggested articles)
- Hindman N, Israel GM. Adrenal gland and adrenal mass calcification. Eur Radiol. 2005 Jun;15(6):1163-7.
- Consul N, Venkatesan AM, Blair KJ, Morshid A, Menias CO, Shaaban AM, Elmohr MM, Gaballah AH, Elsayes KM. Calcified Adrenal Lesions: Pattern Recognition Approach on Computed Tomography With Pathologic Correlation. J Comput Assist Tomogr. 2020 Mar/Apr;44(2):178-187.
Kindly Let Us Know If This Was helpful? Thank You!


