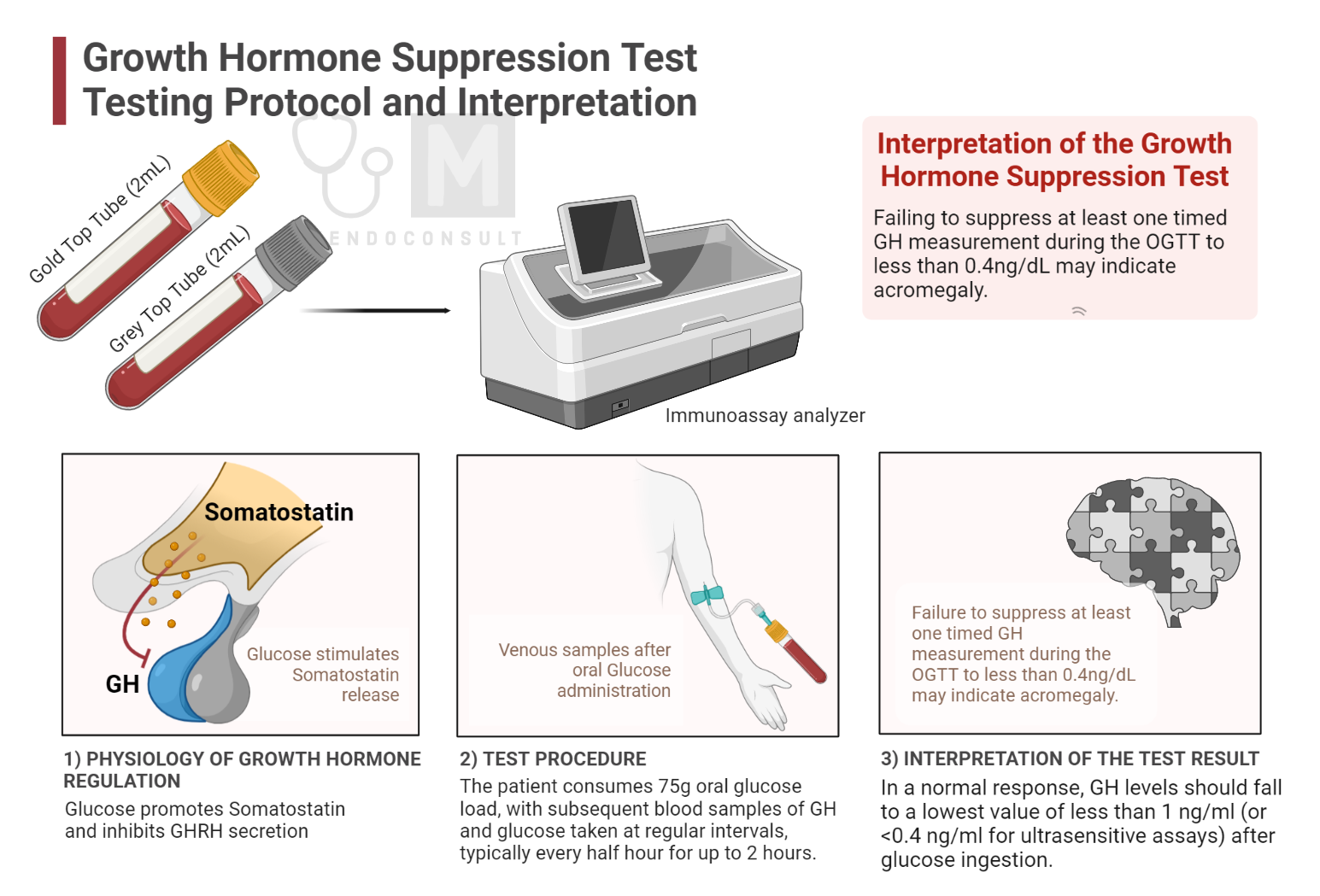
Figure. Growth Hormone Suppression Test. An infographic summarizing the test procedure and interpretation
Indication for the Growth Hormone Suppression Test
The test is intended to confirm the diagnosis of acromegaly in cases where IGF-1 levels are mildly elevated (less than twice the upper limit of normal) and the clinical signs are unclear or absent.
Test Preparation
Preparation: A fasting period of 10 hours is required.
Equipment Required: A 75g of anhydrous glucose, gold-topped and grey-topped tubes.
Method for GH Analysis: An immunoenzymatic assay is used for GH measurement.
Anatomical and Physiological Principles
The growth hormone suppression test, also known as the oral glucose tolerance test (OGTT), is used to assess the inhibition of growth hormone (GH) secretion in patients who may have acromegaly, a condition characterized by excessive GH production and its subsequent effects on the body. This test operates on the physiological principle that glucose intake generally reduces GH secretion in healthy individuals.
In a healthy scenario, an increase in blood glucose levels normally curbs the secretion of GH, resulting in reduced GH levels after glucose intake. However, this inhibitory response is compromised in patients with acromegaly, leading to consistently high or inadequately reduced GH levels after glucose ingestion.
Underlying Mechanisms of the Growth Hormone Suppression Test
The precise way in which glucose suppresses GH secretion has not yet been fully comprehended, but several theories have been put forward to demystify this physiological phenomenon. It is believed that the hypothalamus and anterior pituitary gland, both vital parts of the hypothalamic-pituitary axis overseeing GH secretion, play key roles in this process.
One hypothesis posits that high blood glucose levels trigger the release of somatostatin, also known as growth hormone-inhibiting hormone (GHIH), from the hypothalamus. Somatostatin then acts on the anterior pituitary gland to inhibit GH secretion. This increased release of somatostatin in response to glucose can result in the suppression of GH levels.
Another hypothesis is that elevated blood glucose levels may inhibit the release of growth hormone-releasing hormone (GHRH) from the hypothalamus. GHRH is the stimulant responsible for triggering the release of GH from the anterior pituitary gland. Therefore, inhibiting GHRH release would result in suppressed GH secretion.
There is also a suggestion that glucose may directly inhibit the anterior pituitary gland, thereby decreasing GH secretion. This inhibitory action may involve pituitary somatotroph cells that detect glucose, which in turn could modify intracellular signaling pathways and reduce GH release.
Growth Hormone Suppression Test (Procedure)
The growth hormone suppression test is generally recommended for patients with mild to moderately elevated levels of serum insulin-like growth factor 1 (IGF-1), typically less than twice the upper limit of normal, coupled with inconclusive clinical evidence of excess GH.
The test protocol involves an overnight fast by the patient followed by a baseline blood sample for the initial determination of the GH level. The patient then consumes a 75g oral glucose load, with subsequent blood samples taken at regular intervals, typically every half hour for up to 2 hours. These samples are examined to assess the response of GH levels to oral glucose intake.
In a normal response, GH levels should fall to a nadir of less than 1 ng/ml after glucose ingestion. In patients with acromegaly, GH levels remain high or are not sufficiently suppressed, indicating a malfunctioning feedback mechanism and abnormal GH secretion.
Although the threshold of <1 ng/mL has traditionally been accepted for distinguishing between normal and acromegalic individuals, advances in GH assays have led to revised guidelines proposing a lower diagnostic threshold of 0.4 ng / ml. Thus, failing to suppress at least one timed GH measurement during the OGTT to less than 0.4ng/dL may indicate acromegaly.
References
- Tannenbaum GS, Martin JB (1976) Evidence for an endogenous ultradian rhythm governing growth hormone secretion in the rat. Endocrinology 98:562–570
- Thorner MO, Vance ML, Hartman ML, Holl RW, Evans WS, Veldhuis JD, Van Cauter E, Copinschi G, Bowers CY (1990) Physiological role of somatostatin on growth hormone regulation in humans. Metabolism 39:40–42
- Córdoba-Chacón J, Gahete MD, Culler MD, Castaño JP, Kineman RD, Luque RM (2012) Somatostatin dramatically stimulates growth hormone release from primate somatotrophs acting at low doses via somatostatin receptor 5 and cyclic AMP. J Neuroendocrinol 24:453–463
- Ho KY, Veldhuis JD, Johnson ML, Furlanetto R, Evans WS, Alberti KG, Thorner MO (1988) Fasting enhances growth hormone secretion and amplifies the complex rhythms of growth hormone secretion in man. J Clin Invest 81:968–975
- Hage M, Kamenický P, Chanson P (2019) Growth Hormone Response to Oral Glucose Load: From Normal to Pathological Conditions. Neuroendocrinology 108:244–255
Kindly Let Us Know If This Was helpful? Thank You!

