Vitamin D, also called calciferol, is a fat-soluble compound whose major biological function in humans is maintaining calcium homeostasis. Vitamin D is an umbrella term used to describe two major forms of the molecule, vitamin D2 (ergocalciferol) and vitamin D3 (cholecalciferol). Vitamin D has historically been considered an essential micronutrient. In reference to the definition of a vitamin—a trace dietary component required in small quantities to facilitate critical physiological processes and whose absence in the diet leads to a deficiency state1–3—vitamin D was classified as such.
However, in the past decades, it has widely been referred to by researchers as a hormone, defined as an endogenous chemical substance, produced by glands, that regulates several organ system functions4,5, or prohormone, which is a precursor of a hormone. In contrast, others assert that its active metabolites are the only hormonal forms of vitamin D. Controversy remains regarding the appropriate terminology surrounding this micromolecule.
Understanding the naming system of vitamin D is essential, as the inappropriate labeling of a substance breeds uncertainty and misinformation. Moreover, the importance of applying the appropriate terminology in scientific research and publications cannot be overstated.
Sources and Functions of Vitamin D
Vitamin D is an essential component of a vast array of physiological processes. It occurs naturally in many animal and plant life and can therefore be acquired by human beings through dietary intake. However, most of the vitamin D required by the body is obtained from in vivo synthesis.6–8 While both forms of vitamin D can be sourced from the diet, only vitamin D3 is endogenously synthesized, which occurs by photolysis of its precursor, 7-dehydrocholesterol, upon exposure of human or animal skin to ultraviolet B (UVB) radiation.
Thus, vitamin D3 can be sourced from animal foods (e.g., fatty fish, liver, meat products, and egg yolk) as well as endogenous production. On the other hand, vitamin D2 is synthesized from UVB photolysis of ergosterol found in plants and fungi; its sources include mushrooms and yeast. Dietary supplements and fortified foods like dairy products, juices, and breakfast cereals are other sources of exogenous vitamin D.3,6,9
Although the body can produce vitamin D3, there remains a crucial need for exogenous sources that should not be overlooked, particularly when sufficient sun exposure cannot be attained.3,10
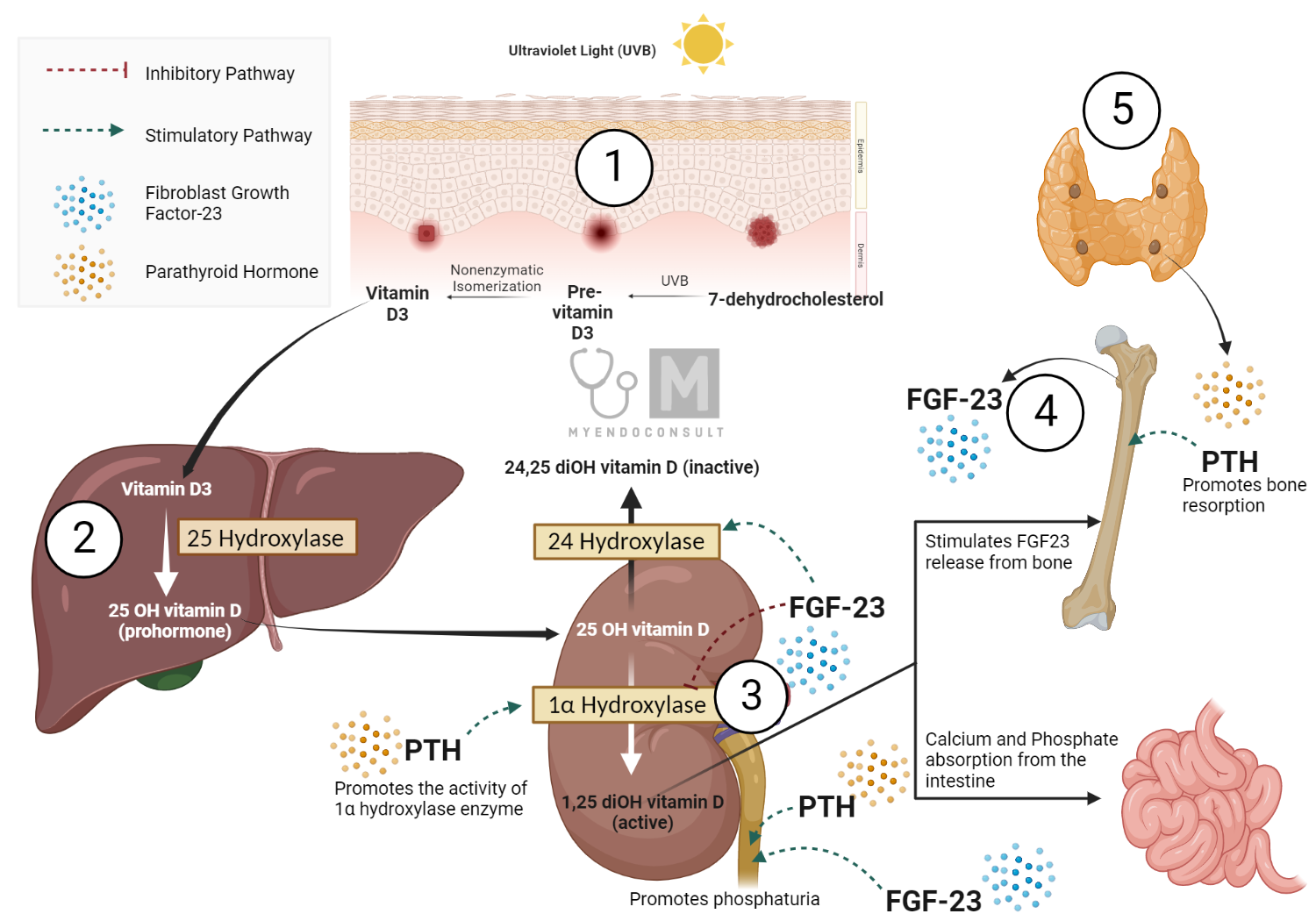
The physiological processes requiring vitamin D are facilitated by its metabolites—25-hydroxyvitamin D (25OHD; calcidiol) and 1,25-dihydroxy vitamin D (1,25(OH)2D; calcitriol). 25OHD is produced when vitamin D undergoes enzymatic hydroxylation, mainly in the liver, while 1,25(OH)2D is obtained from the hydroxylation of 25OHD, primarily in the kidneys. Many organs and tissues, including but not limited to the liver, kidney, skin, muscle, bone, heart, and immune tissue, express the vitamin D receptors, transport proteins and enzymes required to synthesize and mediate the functions of 1,25(OH)2D and generate the appropriate biological responses in the target organ.3,7,11,12 Continued in vivo and in vitro experiments demonstrate the extensive functions of 1,25(OH)2D, both genomic and nongenomic.
Its actions are mediated through interactions with nuclear, cytoplasmic, and cell membrane receptors and include inhibition of cellular proliferation, promotion of cell differentiation, apoptosis, and immune regulation, among others.8–10,13
Furthermore, its potential role in combatting various diseases such as oncologic, cardiovascular, neuromuscular, autoimmune, dermatological, and infectious conditions has received considerable attention and continues to be studied. The presence of vitamin D receptors in several tissues supports the claims of its role, or potential role, in maintaining organ function and preventing disease.
The functions and potential actions of vitamin D metabolites are largely demonstrated through research encompassing various vitamin D deficiency states such as rickets, osteomalacia, and osteoporosis. The role of vitamin D in calcium and phosphate regulation and bone metabolism is well-established. 1,25(OH)2D maintains the serum levels of calcium and phosphate within a normal narrow range by promoting intestinal calcium and phosphate absorption, mobilizing calcium from bones through resorption, and stimulating renal reabsorption of calcium and phosphate.10,11
Vitamin D-dependent calcium homeostasis is further enhanced by the parathyroid hormone, which upregulates the serum levels of 1,25(OH)2D.6,8 By maintaining calcium and phosphate homeostasis, two vital elements of bone mineralization, 1,25(OH)2D supports bone development and skeletal health. In addition, it promotes bone maturation, matrix formation, and remodeling.10
Its role in controlling infectious and autoimmune disease processes is attributable to its immune-modulating actions. 1,25(OH)2D is known to inhibit antigen presentation by dendritic cells, antibody production by B lymphocytes, and proliferation of T and B lymphocytes, and enhance the effects of T suppressor lymphocytes; this confers a tolerogenic effect and prevents overexpression of the immune response. It also influences T-cell differentiation, amplifies the antimicrobial action of macrophages and monocytes, and increases chemotaxis, autophagy, and phagolysosomal fusion, thus protecting against infections.11,13–15
Another area of interest in research is the association between vitamin D and cancer. The inhibitory action of 1,25(OH)2D in the evolution of certain cancers and hyperproliferative disorders, including leukemia, breast cancer, colorectal cancer, and prostate cancer, has been explained by cellular proliferation inhibition, anti-angiogenic action, and apoptotic properties.6,10,11,14
In dermatology, 1,25(OH)2D is used to treat psoriasis, melanoma, and scleroderma; this is thought to be mediated by its immunosuppressive, differentiation-inducing, and anti-proliferative properties in the skin.13,14 Other actions of 1,25(OH)2D that have been explored are control of muscular and nervous system function, protection against cardiovascular disease, and maintenance of obstetric health.6,7,10,14
Defining what hormones are
Hormones are chemical messenger molecules produced by both plants and animals to regulate cellular activity and maintain a homeostatic environment.4,5 In the human body, they are synthesized by various glands (hypothalamus, pituitary, thyroid, adrenal gland, etc.) and other specialized cells. They are released into the bloodstream, bound to transport proteins, and carried to their target organs, where they elicit a biological response.
Others act locally by interacting with receptors on neighboring cells, the secreting cell, or within the secreting cell. Thus, hormones exhibit endocrine, paracrine, autocrine, and intracrine properties, and a single hormone can influence multiple organ functions.16
A deficit in hormone production will lead to a deficiency state characterized by the absence of physiological processes elicited by the hormone, and, as many organs can be influenced by one hormone, multiple organ systems may be affected.
The hormones formed by the body are numerous and have been categorized by many classification systems. Based on their chemical nature, they are grouped into protein, steroid, and eicosanoid hormones, derived from amino acids, cholesterol, and arachidonic acid, respectively.16,17
Hormones effect biological responses by binding to their receptors on the surface of or within target cells and modifying cellular activity, thus triggering responses such as the synthesis of new molecules, metabolic actions, gene modification (steroid hormones), or alteration of the permeability of the cell membrane.17,18
Hormones regulate metabolism, differentiation, growth and development of organs, immune function, blood pressure control, reproduction, and nervous system function, to mention a few.19
Vitamin D as a Hormone
Vitamin D was discovered in the early 1900s based on a multitude of studies on the causes and management of rickets and was classified as a nutrient.1,3,7,20 Experimental studies demonstrating its hormone-like activity and structural composition led to its reclassification as a hormone.1,21
Vitamin D has been shown to possess a closely similar molecular morphology as other steroid hormones such as cortisol, progesterone, and estradiol.1,7,13,22 Like hormones, it is produced by specialized cells and released into the bloodstream to elicit physiological responses in distant target organs and, in addition, possess local paracrine, intracrine, and autocrine functions.
Its active metabolites have been proven to exhibit a mechanism of action analogous to hormones; they can cross the cell membrane to interact with their specific nuclear receptors leading to gene modification (genomic responses) and cell surface receptors to induce signaling pathways through the production of cellular messengers (nongenomic responses).7
The autoregulation of vitamin D serum levels through a feedback loop by calcium serum concentration and parathyroid hormone and the development of a deficiency disease when unavailable in sufficient amounts further meets the criterion of a hormone.21,23
In recent years, several literary publications have asserted that the term vitamin D is a misnomer since the molecule is not a true vitamin in the sense that it can also be derived through endogenous synthesis.2,3,7,24,25 The implication is that it can be described as a vitamin only when conditions inhibit its production by the body.
Some researchers have recommended that specific terms must be used to describe the two forms of vitamin D, i.e., vitamins D3 and D2, and the term vitamin D not be inaccurately used to describe the hormone 1,25(OH)2D.2,26 There is a wide consensus that vitamin D is a steroid precursor required for the production of its hormone derivative, 1,25(OH)2D.
Conclusion
Vitamin D is a vital micromolecule that is both a dietary constituent and an endogenous substance formed in the skin. It produces vast biological responses, primarily in the regulation of calcium metabolism. It exerts its functions through 1,25(OH)2D, which interacts with the vitamin D receptor to regulate specific cellular activity. Vitamin D and steroid hormones are known to have a similar chemical structure. Furthermore, steroid hormones and the metabolites of vitamin D exhibit similar mechanisms by which they exert their functions, both acting through their cell surface and intracellular receptors and producing similar effects on cellular physiology.
In contrast to hormones, however, vitamin D can be obtained through dietary intake. Referencing the enormous body of scientific literature on vitamin D, it is suitable to say that vitamin D is a prohormone, whereas its active metabolite is a hormone. Classifying vitamin D as a hormone conveys that it is not essentially needed in the diet as it is synthesized in the body. However, this may, at the same time, result in an underestimation of the need for exogenous vitamin D.
References
- Norman AW. The History of the Discovery of Vitamin D and Its Daughter Steroid Hormone. Ann Nutr Metab [Internet]. 2012;61(3):199–206. Available from: 1159/000343104
- Vieth R. Vitamin D supplementation: cholecalciferol, calcifediol, and calcitriol. Eur J Clin Nutr [Internet]. 2012;74(11):1493–7. Available from: 1038/s41430-020-0697-1
- Jones G. 100 YEARS OF VITAMIN D: Historical aspects of vitamin D. 2022;11(4). Available from: 1530/ec-21-0594
- Barrington EJW. Hormone [Internet]. Encyclopedia Britannica. 2022 [cited 2023 Feb 21]. Available from: https://www.britannica.com/science/hormone
- Sandow J. Hormones, 1. Hormone Systems. 2011 [cited 2023 Feb 22]; Available from: 1002/14356007.a13_089.pub2
- Borradale D, Kimlin M. Vitamin D in health and disease: an insight into traditional functions and new roles for the ‘sunshine vitamin.’ Nutr Res Rev [Internet]. 2009;22(2):118–36. Available from: 1017/s0954422409990102
- Monastra G, De Grazia S, De Luca L, Vittorio S, Unfer V. Vitamin D: a steroid hormone with progesterone-like activity. Eur Rev Med Pharmacol Sci [Internet]. 2018;22(8):2502–12. Available from: 26355/eurrev_201804_14845
- Vijay K, Pallavi S, Yashank Y, Rakesh T. Role Of Vitamin D In Health And Diseases In Children. Indian J Pediatrics . 2015;4(4).
- Pfotenhauer KM, Shubrook JH. Vitamin D Deficiency, Its Role in Health and Disease, and Current Supplementation Recommendations. 2017;117(5):301–5. Available from: 7556/jaoa.2017.055
- Craveiro V, Araújo J, Santos A, Ramos E. Vitamin D – from the pro-hormone to the biological actions. Acta Port Nutr [Internet]. 2019;19. Available from: 21011/apn.2017.1909
- Bikle DD. Vitamin D: an ancient hormone. Experimental Dermatology [Internet]. 2011;20(1):7–13. Available from: 1111/j.1600-0625.2010.01202.x
- Holick MF. Vitamin D Deficiency. N Engl J Med [Internet]. 2007;357(3). Available from: https://doi.org/10.1056/nejmra070553
- Reichrath J, Lehmann B, Carlberg C, Varani J, Zouboulis C. Vitamins as Hormones. Horm Metab Res [Internet]. 2007;39(2):71–84. Available from: 1055/s-2007-958715
- Dusso AS, Brown AJ, Slatopolsky E. Vitamin D. American Journal of Physiology-Renal Physiology [Internet]. 2005;289(1):F8–28. Available from: 1152/ajprenal.00336.2004
- Sassi F, Tamone C, D’Amelio P. Vitamin D: Nutrient, Hormone, and Immunomodulator. Nutrients [Internet]. 2018 [cited 2023 Feb 22];10(11):1656. Available from: 3390/nu10111656
- Johnstone C, Hendry C, Farley A, McLafferty E. Endocrine system: part 1. Nursing Standard [Internet]. 2014 [cited 2023 Feb 22];28(38):42–9. Available from: 7748/ns.28.38.42.e7471
- McLaughlin MB. Biochemistry, Hormones [Internet]. StatPearls Publishing; 2022 [cited 2023 Feb 22]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK541112/
- McEwen BS. Classification of Hormonal Effects. In: Basic Neurochemistry: Molecular, Cellular and Medical Aspects [Internet]. 6th ed. Philadelphia: Lippincott-Raven; 2022 [cited 2023 Feb 22]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK28055/
- Campbell M, Jialal I. Physiology, Endocrine Hormones. StatPearls [Internet]. 2022 [cited 2023 Feb 22]; Available from: https://www.ncbi.nlm.nih.gov/books/NBK538498/
- Norman AW. Vitamin D Receptor: New Assignments for an Already Busy Receptor. Endocrinology [Internet]. 2006;147(12):5542–8. Available from: 1210/en.2006-0946
- Norman AW. The Hormone-like Action of 1,25-(OH)2-Cholecalciferol (A Metabolite of the Fat-Soluble Vitamin D) in the Intestine. Vitam Horm [Internet]. 1975 [cited 2023 Feb 22];325–84. Available from: 1016/s0083-6729(08)60018-7
- Ellison DL, Moran HR. Vitamin D: Vitamin or Hormone? Nursing Clinics of North America [Internet]. 2021;56(1):47–57. Available from: 1016/j.cnur.2020.10.004
- Deluca HF. Vitamin D as a prohormone. Biochemical Pharmacology [Internet]. 1977;26(7):563–6. Available from: 1016/0006-2952(77)90025-9
- Demer LL, Hsu JJ, Tintut Y. Steroid Hormone Vitamin D. Circ Res [Internet]. 2018;122(11):1576–85. Available from: 1161/circresaha.118.311585
- Vojinovic J, Cimaz R. Vitamin D—update for the pediatric rheumatologists. Pediatr Rheumatol [Internet]. 2015;13(1). Available from: 1186/s12969-015-0017-9
- Norman AW. From vitamin D to hormone D: fundamentals of the vitamin D endocrine system essential for good health. The American Journal of Clinical Nutrition [Internet]. 2008;88(2):491S-499S. Available from: 1093/ajcn/88.2.491s


