Follicular carcinoma is the second most common type of thyroid cancer, accounting for approximately 10-15% of all cases. It arises from the follicular cells of the thyroid gland and is generally more aggressive than papillary thyroid carcinoma. In this review, we will provide a detailed description of the histological features of follicular carcinoma and outline the features of vascular and capsular invasion.
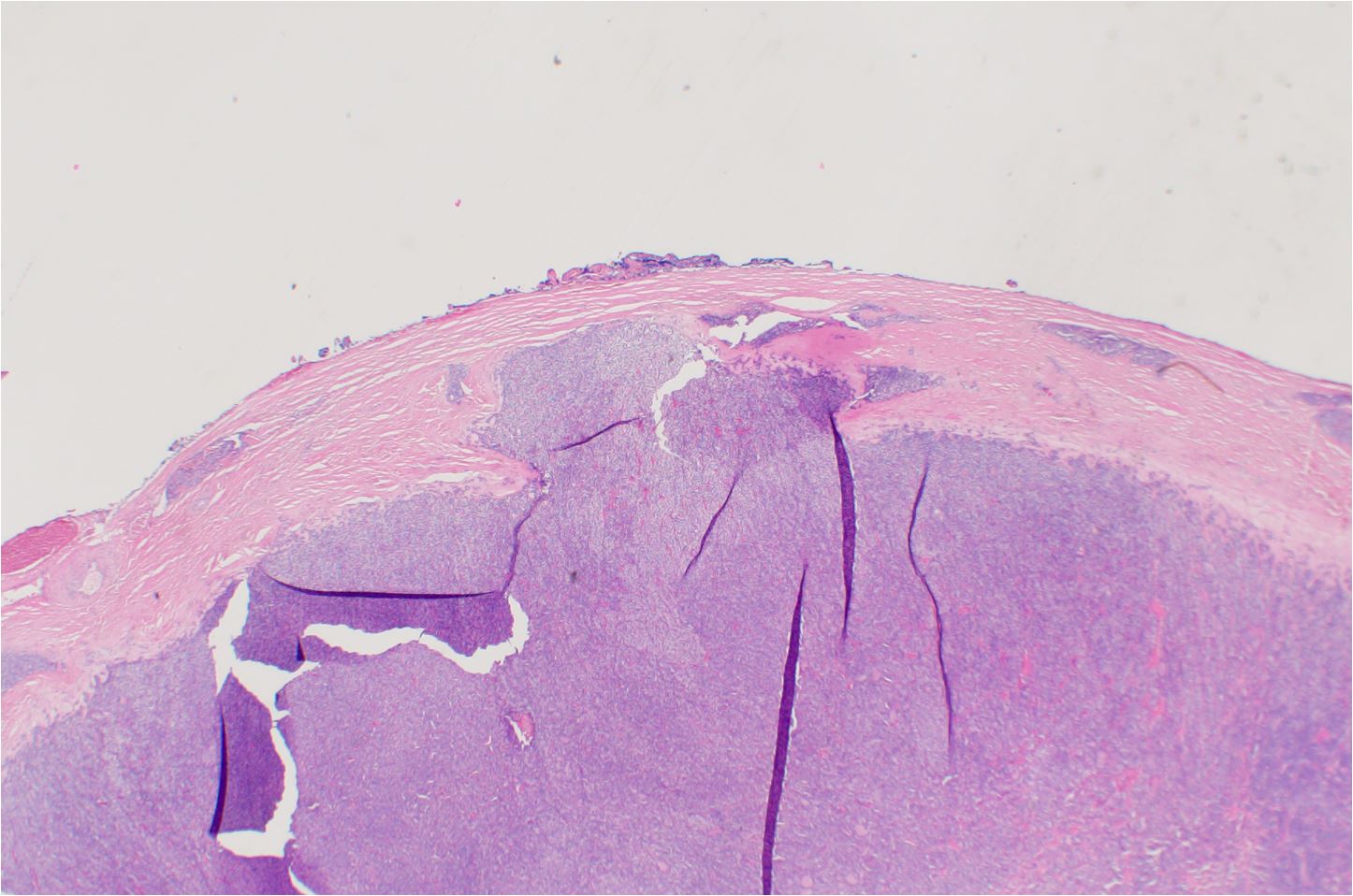
Follicular carcinoma with capsular invasion (click image to enlarge). Follicular carcinoma with a focus of capsular invasion. Note the presence of a thick capsule. Capsular invasion often presents with mushroom like invasion into and even through the capsule
Histological features of follicular carcinoma of the thyroid
- Gross appearance: Follicular carcinomas are typically well-circumscribed, round to oval, encapsulated masses that may vary in size. Furthermore, the cut surface may appear solid, partially cystic, or filled with colloid material. Tumors can range from tan to pale yellow or brown and may exhibit areas of hemorrhage or necrosis.
- Cellular architecture: Follicular carcinoma is characterized by a predominantly follicular growth pattern, with cells arranged in a microfollicular, trabecular, or solid pattern. Indeed, these patterns can be admixed in various proportions within the tumor. The follicles may be smaller, more irregular, and tightly packed compared to normal thyroid follicles.
- Cellular morphology: The neoplastic cells in follicular carcinoma resemble normal thyroid follicular cells but may exhibit varying degrees of nuclear and cellular atypia. The cells are typically cuboidal or columnar with an increased nucleus-to-cytoplasm ratio, and the cytoplasm may be eosinophilic or clear due to the presence of glycogen or lipid. Nuclear pleomorphism, hyperchromasia, and prominent nucleoli may be observed, although these findings are generally less prominent than in papillary thyroid carcinoma.
- Capsular invasion: Capsular invasion is a critical diagnostic feature of follicular carcinoma. It refers to the infiltration of tumor cells through the capsule that surrounds the tumor mass. Histologically, capsular invasion can be observed as tumor cells breaching the capsule and extending into the surrounding thyroid parenchyma or fibrous tissue. This attribute distinguishes follicular carcinoma from follicular adenoma, which is a benign encapsulated tumor without capsular or vascular invasion.
- Vascular invasion: Vascular invasion is another important diagnostic criterion for follicular carcinoma. It is identified by the presence of tumor cells within the endothelium-lined spaces of blood vessels within or immediately adjacent to the tumor capsule. Vascular invasion is a marker of more aggressive behavior and is associated with an increased risk of metastasis, particularly to the lungs and bones.
- Mitotic activity: Follicular carcinomas may exhibit an increased mitotic rate compared to normal thyroid follicular cells. However, the mitotic activity may not be as high as in other aggressive thyroid cancers, such as anaplastic carcinoma.
- Necrosis: Areas of tumor necrosis may be present in follicular carcinoma, particularly in larger or more aggressive tumors.
- Lymphatic invasion and lymph node involvement: In contrast to papillary thyroid carcinoma, follicular carcinoma is less likely to exhibit lymphatic invasion or lymph node metastasis. Hematogenous spread is more common in this type of thyroid cancer.
H and E staining of Follicular Carcinoma of the Thyroid
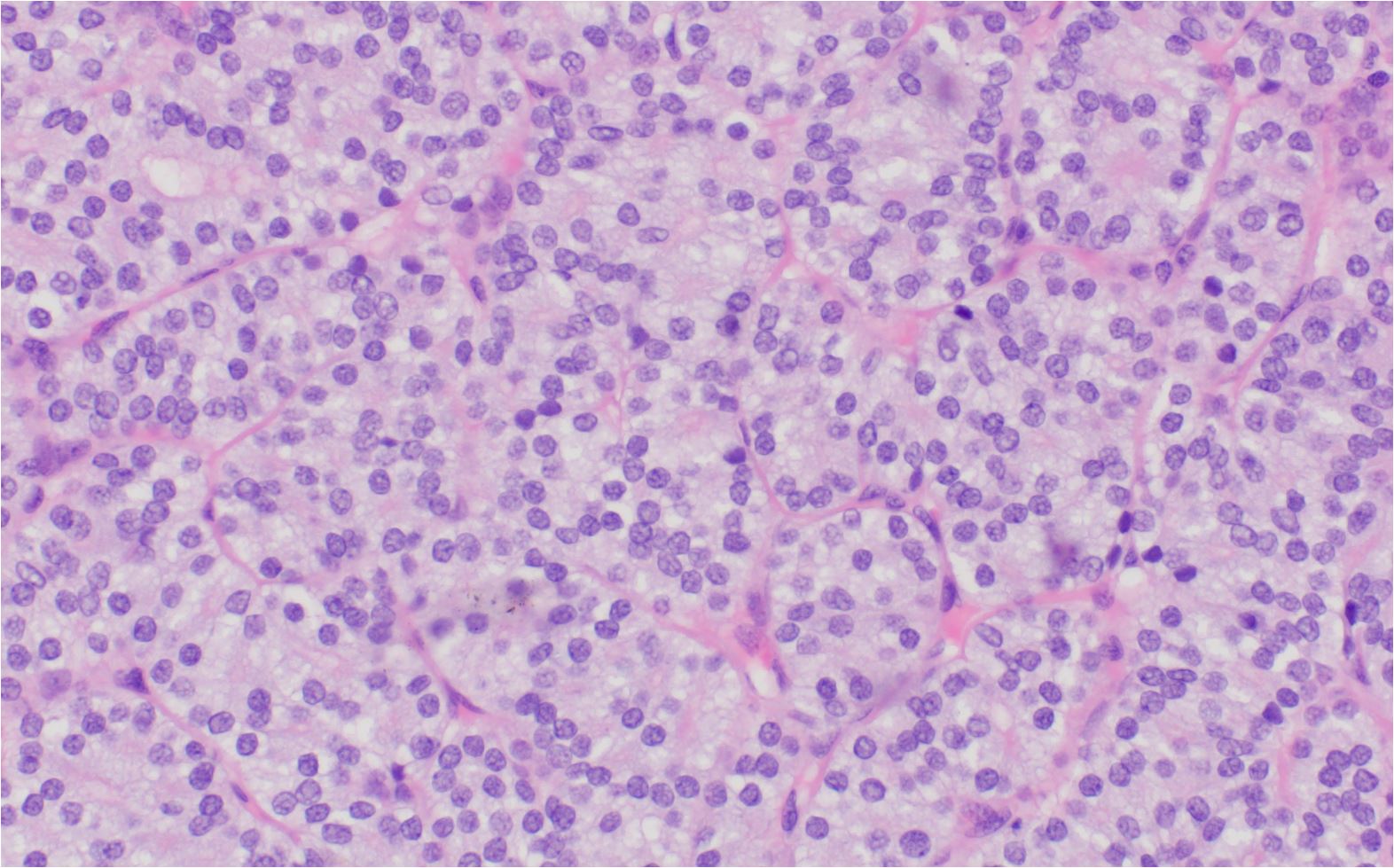
Follicular carcinoma of the thyroid gland (high magnification). Follicular carcinoma high magnification showing the microfollicular syncytial architecture. Mild cytologic atypia including nuclear enlargement
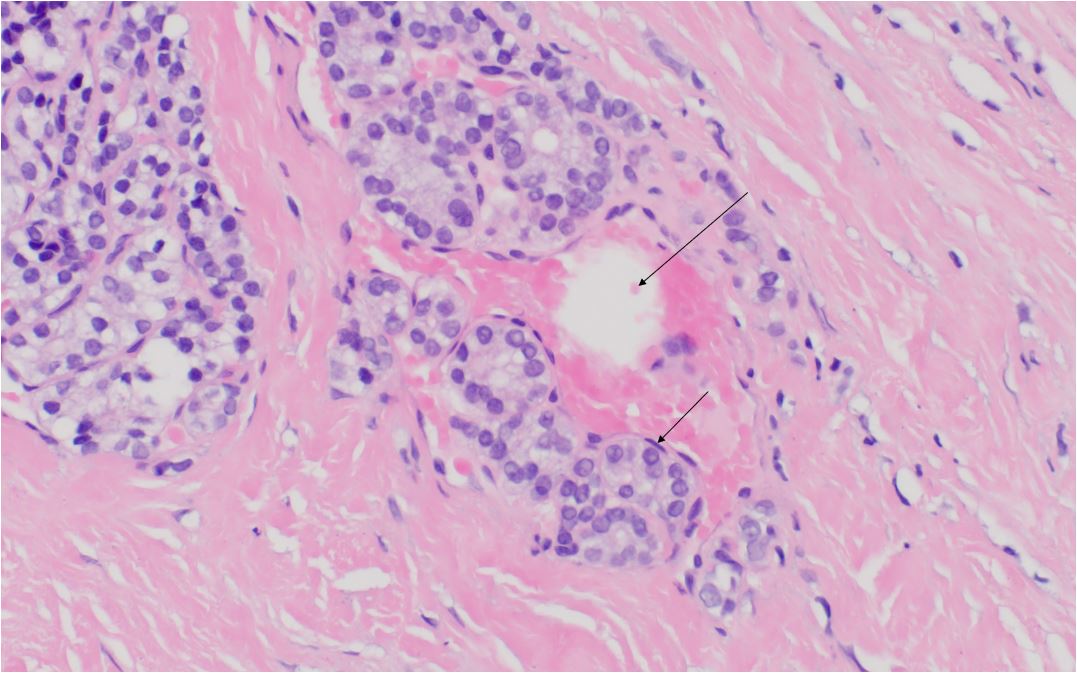
Follicular carcinoma with vascular invasion. Vascular lumen (long arrow) Endothelial cells lining tumor within vessel (short arrow)
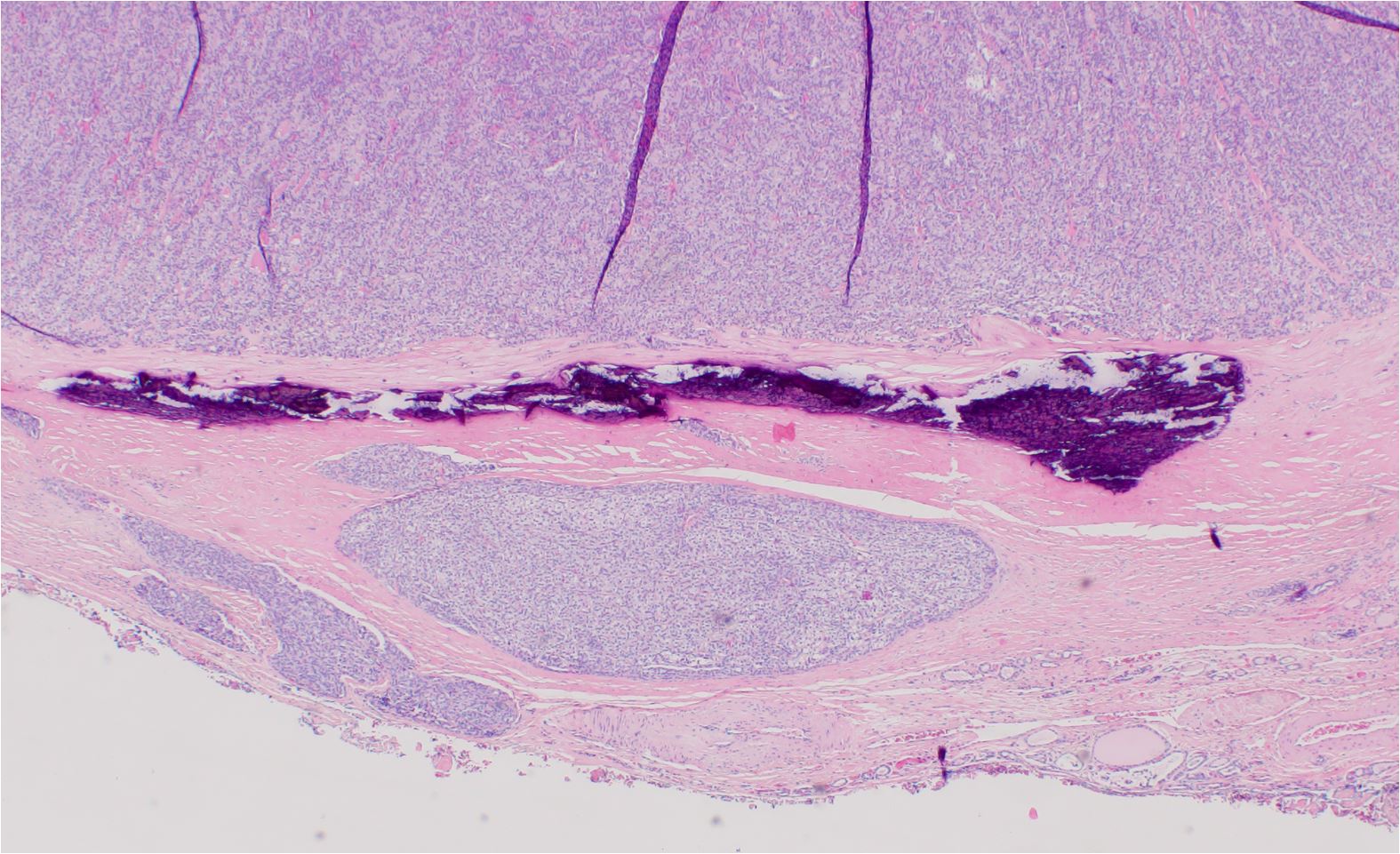
Follicular carcinoma of the thyroid with capsular invasion. There is capsular invasion within thick capsule. Deeper sections could show connection
In summary, follicular carcinoma is characterized by a predominantly follicular growth pattern, varying degrees of nuclear and cellular atypia, and the presence of capsular and/or vascular invasion. The identification of capsular and vascular invasion is crucial in distinguishing follicular carcinoma from benign follicular adenoma and predicting the tumor’s clinical behavior.
Kindly Let Us Know If This Was helpful? Thank You!


