
PCOS is characterized by amenorrhea/oligomenorrhea, hirsutism, acne, and infertility among women in the reproductive age group. The underlying pathophysiology of PCOS will be reviewed (refer to a comprehensive review of PCOS pathophysiology here). Also, the pathophysiologic basis of various clinical features of this condition is discussed next.
Hirsutism
Clinical features
Hirsutism is defined as the presence of terminal, pigmented hair in a male-pattern distribution. It is a common dermatologic manifestation of polycystic ovary syndrome (PCOS) with a reported prevalence of 50-70%.
Pathophysiology
Circulating androgens are responsible for hirsutism, although the degree of hirsutism is not necessarily determined by the severity of hyperandrogenemia. This has been attributed to interindividual differences inthe response of hair follicles to androgens.
Hirsutism, like acne, and male pattern alopecia is dependent on the local abundance of 5-α-reductase(which reduces testosterone to active dihydrotestosterone) in the pilosebaceous unit.
The local concentration of 5-α-reductase in the skin varies by ethnicity. For example, hirsutism tends to be more common in women of Mediterranean background and less frequent and milder in women of East Asian or Native-American background.
Acanthosis nigricans
Clinical features
Acanthosis nigricans (AN) is a classic dermatologic manifestation of PCOS and other endocrinopathies associated with insulin resistance. It is a velvety, dark, and plaque-like skin lesion with a predilection for flexural areas such as the neck and axillary regions. 50% of patients with the classic obese PCOS phenotype have AN.
Pathophysiology
Hyperinsulinemia stimulates keratinocytes and fibroblasts directly, leading to their proliferation. Additional mechanisms accounting for hyperinsulinemia-induced hirsutism have been described earlier.
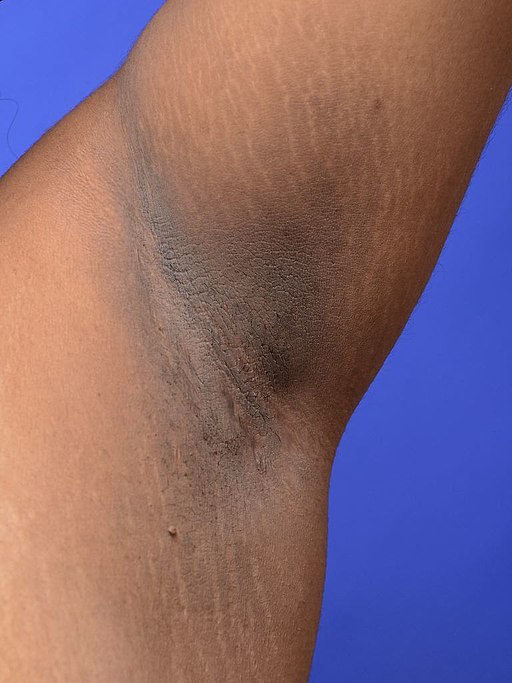 Mark F. Brady; Prashanth Rawla., CC BY-SA 4.0
Mark F. Brady; Prashanth Rawla., CC BY-SA 4.0Acne
Clinical features
Acne is a common skin manifestation of PCOS, with a highly variable prevalence, based on ethnicity. Asian Indians have the highest prevalence, with the lowest being among Pacific Islanders.
Pathophysiology
- Hyperinsulinemia in the setting of PCOS potentiates the excretion of sebum through the effects of insulin acting on IGF-1 receptors present on sweat glands. Accumulation of sebum establishes a milieu conducive for the proliferation of Propionibacterium acnes and the eventual formation of comedones.
- Dihydrotesterone (an androgen) binds to its receptors on sweat glands and influences their output of sebum, as well. Interestingly, the severity of acne is not dependent on the degree of hyperandrogenemia and may be due to the variable sensitivity of pilosebaceous units to circulating androgens.
 Diariodaj, Public domain, via Wikimedia Commons
Diariodaj, Public domain, via Wikimedia CommonsObesity
Clinical features
The prevalence of obesity in patients with PCOS is between 40 to 80%. In contrast to women outside the United States(US), PCOS patients in the US have relatively higher body mass indexes (BMI’s).
Pathophysiology
Circulating levels of androgen influence the distribution of body fat. Men have higher levels of testosterone, and as such, have a higher concentration of fat in the central abdomen compared to the hips or lower body. Women with PCOS have high levels of testosterone, which changes the typical gynoid fat distribution into an android one. This is the reason for increased central or visceral adiposity.
More recent evidence refutes this hypothesis in women with PCOS. Although obese and non-obese women with PCOS had high levels of androgens compared to matched controls without PCOS, there was no difference in visceral adiposity between these two groups of PCOS subjects in this study. The mechanisms remain incompletely understood at this time.
Pathophysiology of PCOS
 Schematic representation of the pathophysiology of PCOS
Schematic representation of the pathophysiology of PCOS1) Increased activity of the GnRH pulse generator stimulates central gonadotrophs and results in an increase in luteinizing hormone (LH) with a concomitant decrease in follicle-stimulating hormone (FSH).
2) LH stimulates theca cells of the ovaries to produce testosterone. Low FSH, on the other hand, results in less stimulation of the granulosa cell-mediated conversion of theca cell derived-testosterone into estrogens.
3) Reduced levels of circulating sex hormone-binding globulin (SHBG) worsens the degree of hyperandrogenemia, as well. Both hyperandrogenemia and hyperinsulinemia impair hepatic SHBG synthesis, and since SHBG binds more avidly to estrogens than it does androgens, low levels of circulating SHBG increases the free androgen to free estrogen ratio.
4) Hyperandrogenemia impairs negative feedback effects of estrogen on the pituitary gonadotrophs, which results in unimpaired LH release and maintenance of a vicious cycle of hyperandrogenemia.
5) Adrenal-derived androgens play a contributory role, although the mechanisms are incompletely understood.
Questions
Pathophysiology of PCOS usmle or endocrine board review preparation.
What are the reasons for insulin resistance in patients with PCOS?
- Post insulin to insulin-receptor binding defects contributes to insulin resistance in patients with PCOS.
- Reduction in glucose transporter 4 (GLUT-4) receptors in adipose tissue lead to reduced glucose uptake.
- Persistent hyperglycemia promotes rebound and persistent hyperinsulinemia. A prolonged period of hyperinsulinemia leads to progressive beta-cell dysfunction and death.
- Androgens may play a modest role in insulin resistance, although elevated serum androgens alone cannot explain insulin resistance in PCOS.
- Co-morbid dyslipidemia contributes to lipotoxicity-induced insulin resistance.
- There is also an increase, partially obesity-related, in inflammatory adipokines such as tumor-necrosis-factor-alpha (TNF-α), which induces insulin resistance. Furthermore, there is a concomitant decrease in the insulin-sensitizing adipokine, adiponectin.
What conditions should be ruled out as part of the evaluation of PCOS?
Hypothyroidism, prolactinoma, nonclassical congenital adrenal hyperplasia, Cushing’s syndrome, androgen-secreting tumor, and acromegaly.
Also, it is prudent to rule out pregnancy, primary ovarian insufficiency, or functional hypothalamic amenorrhea in select patients based on the clinical presentation. It should go without saying that pregnancy must always be excluded in any woman of reproductive age with amenorrhea.
Which endocrine conditions are associated with hirsutism/virilization apart from PCOS?
The features of virilization include acne, male pattern baldness, deep male voice, and clitoral enlargement
- Adrenal tumors
- Cushing’s syndrome
- Classic and non-classic congenital adrenal hyperplasia
- Hyperandrogenism, insulin resistance, acanthosis nigricans (HAIR-AN syndrome)
- Ovarian hyperthecosis
- Ovarian tumors
Selected References
- Baskind NE, Balen AH (2016) Hypothalamic-pituitary, ovarian and adrenal contributions to polycystic ovary syndrome. Best Pract Res Clin Obstet Gynaecol 37:80–97
- Dunaif A (1997) Insulin resistance and the polycystic ovary syndrome: mechanism and implications for pathogenesis. Endocr Rev 18:774–800
Image(s) Courtesy
MyEndoConsult
Kindly Let Us Know If This Was helpful? Thank You!


