
Thyroid disease is a complex and often misunderstood condition that can have significant impacts on an individual’s physical and mental health. If you or someone close to you has been diagnosed with thyroid disease, it’s important to know the facts so that proper treatment options can be explored.
In this comprehensive guide for patients, we’ll cover symptoms of thyroid diseases, diagnosis methods, treatments available, how to manage living with the condition as well as resources for further support. Thyroid disease – a comprehensive guide for patients – let’s get started!
Symptoms of Thyroid Disease
Thyroid disease is a condition that affects the thyroid gland, which is responsible for producing hormones that regulate metabolism and other bodily functions. Symptoms of thyroid disease can vary depending on the type of disorder present, but some common signs include fatigue, weight gain or loss, changes in mood or energy levels, difficulty sleeping, dry skin, and hair loss.
In hypothyroidism (underactive thyroid), symptoms may include extreme tiredness; feeling cold when others are not; constipation; depression; thinning hair; dry skin and nails; muscle aches and stiffness; slow heart rate; memory problems or forgetfulness.
Hyperthyroidism (overactive thyroid) may cause increased appetite with weight loss despite eating more than usual; rapid heartbeat or palpitations (feeling like your heart is pounding); anxiety or irritability along with restlessness and difficulty sleeping at night due to racing thoughts. Other symptoms can include bulging eyes caused by Graves’ Disease as well as tremors in the hands.
Goiter – an enlargement of the neck due to an enlarged thyroid gland – can be another symptom of both hypo-and hyperthyroidism. Patients with goiters can develop a myriad of local compressive symptoms such as difficulty with breathing, discomfort in swallowing, or a pressure sensation in the neck. If there is significant enlargement of the thyroid gland, important nerves and blood vessels may be compressed, leading to additional symptoms.
Some patients may develop significant reddening of the face when they raise their arms up – this is known as Pemberton’s sign. Paralysis of cranial nerves involved in the proper function of the eye (Horner’s syndrome) and diaphragm can also occur.
It is important to note that many individuals who have a mild form of one type of thyroid disorder may not show any obvious signs at all, while those who have more severe cases will often display multiple symptoms from both types simultaneously. If you suspect you might have a problem with your thyroid, it is best to speak with your doctor about getting tested so they can determine what kind of treatment plan would be most beneficial for you based on your individual needs and health history.
It is important to be aware of the signs and symptoms of thyroid disease, so that appropriate diagnosis and treatment can be sought. Next, we will discuss how thyroid disease is diagnosed.
Key MessageThyroid disease can cause a range of physical and emotional symptoms, including fatigue, weight gain or loss, changes in mood, energy levels, dry skin, hair loss, goiter, and anxiety/depression. If you suspect you may have a problem with your thyroid, it is important to speak with your doctor for proper diagnosis and treatment.
Diagnosis of Thyroid Disease
Blood Tests
Blood tests are a key part of diagnosing thyroid disease. Thyroid stimulating hormone (TSH) is the most commonly used test to measure how well the thyroid is functioning. If TSH levels are too high, it may indicate an underactive thyroid or hypothyroidism; if TSH levels are too low, it could mean an overactive thyroid or hyperthyroidism. These are general rules for primary thyroid dysfunction (disorder of the thyroid gland). TSH levels will, however be different in those with central thyroid dysfunction (mainly at the level of the pituitary gland or hypothalamus).
For example, patients with central hypothyroidism will have either a low or normal TSH level. An understanding of thyroid hormone physiology is required in order to better appreciate the complex relationship between TSH and thyroid hormone levels.
Other blood tests can be used to measure hormones produced by the thyroid and antibodies that can cause inflammation in the gland. For example, thyroglobulin antibody and Thyroid peroxidase antibody may be positive in patients with Hashimoto’s disease (primary hypothyroidism).
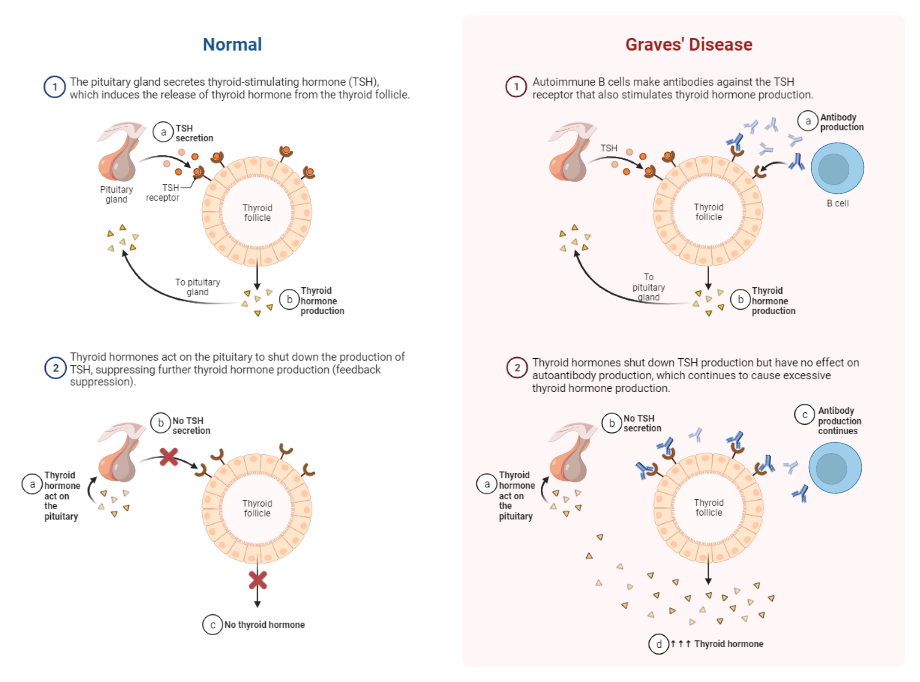
Thyroid stimulating immunoglobulin (TSI) is positive in Graves disease (hyperthyroidism associated with a diffusely enlarged thyroid gland).
Imaging Scans
Imaging scans such as ultrasound and computed tomography (CT) scans can also be used to diagnose thyroid conditions. These scans help doctors identify any lumps or nodules on the gland, which could indicate cancerous growths or other issues with its function.
Ultrasound images provide detailed information about the size, shape, and echo pattern of these lumps while CT scans create cross-sectional images of internal organs in relation to the thyroid gland. CT scans can help identify significant compression of nerves or major blood vessels close to the thyroid gland.
Interpreting Test Results
Once all necessary tests have been completed, doctors will interpret the results to make a diagnosis of either hypo- or hyperthyroidism based on their findings from both blood work and imaging studies. Depending on what type of condition is present, treatment options will vary accordingly; for example, medications may be prescribed for hypothyroidism, while radioactive iodine or surgery might be recommended for hyperthyroidism cases caused by Graves’ Disease.
Treatment Options for Thyroid Disease
Thyroid disease is a common condition that affects millions of people worldwide. Treatment options vary depending on the type and severity of the condition, but may include medications, lifestyle changes, or surgery.
Medications: Medication is often used to treat thyroid disease. Common medications for hypothyroidism (underactive thyroid) are levothyroxine and liothyronine which help replace hormones your body can’t make naturally. Thyroid hormone replacement therapy is identical to the hormone produced by the human body. Theoretically, a well monitored therapy should not cause any side effects. However, in some cases, patients may develop an allergic reaction to excipients (agents for maintaining thyroid hormone in a pill form).
For hyperthyroidism (overactive thyroid), antithyroid drugs such as methimazole or propylthiouracil are typically prescribed to reduce hormone production in the gland.
Side effects from these medications may include nausea, vomiting, headaches, insomnia, and skin rash.
Making simple lifestyle changes can also help manage symptoms of thyroid disease such as fatigue and weight gain/loss associated with an underactive or overactive gland, respectively.
These changes might include eating a healthy diet full of fruits and vegetables; exercising regularly; getting enough sleep; managing stress levels; avoiding caffeine and alcohol; avoiding so-called “thyroid support supplements” sold by unscrupulous websites, and avoiding certain foods that contain goitrogens (substances that interfere with the normal functioning of the thyroid).
In some cases where medication does not work or when there is an underlying tumor causing problems with hormone production, surgery may be recommended by your doctor to remove part or all of the affected gland(s). Surgery carries risks, including infection at the incision site, damage to surrounding tissue/organs during the removal process, and bleeding during the procedure.
Treatment options for thyroid disease can vary depending on the severity and type of condition, so it is important to work with a medical professional to develop an individualized plan. Next, we will discuss how to best manage living with thyroid disease.
Living with Thyroid Disease
Living with thyroid disease can be challenging, but there are ways to manage it. Eating a healthy diet is essential for managing thyroid disease. Foods rich in iodine and selenium, such as seafood, eggs, and dairy products, are not necessary for people with thyroid disease. There are a lot of websites recommending these supplements. The truth is that, they are almost always never needed.
Furthermore, avoiding processed foods and refined sugars is also essential for maintaining your general health. Regular exercise may help keep symptoms under control by improving circulation and reducing stress levels.
Managing emotions associated with having a chronic condition like thyroid disease is also important. It’s normal to feel overwhelmed or frustrated at times; however, seeking support from family members or friends can provide emotional relief during difficult times.
Additionally, talking to a mental health professional about any feelings of depression or anxiety may be beneficial for some people living with thyroid disease.
Staying organized when taking medications is key to successfully managing the condition. Keeping track of medication schedules on an app or calendar will help ensure that doses are taken on time each day without missing any doses, which could lead to complications down the road if not managed properly over time.
Additionally, staying up-to-date on research related to treatment options available for your specific type of thyroid disorder will help you make informed decisions about your care plan moving forward.
People with thyroid disease can also have other medical conditions which may masquerade as thyroid disease. Fatigue may be due to anemia (low blood level), undiagnosed obstructive sleep apnea, adrenal insufficiency, or even depression. Assuming that all of your symptoms are solely due to thyroid disease can lead to inappropriate and likely harmful treatment. The recent trend of patients insisting on multiple blood tests and frequent adjustments in medications has led, in some cases, to unintended consequences.
Living with thyroid disease can be a difficult and challenging experience, but it is important to remember that you are not alone. There are many resources available to help manage your condition and improve your quality of life. Now let’s explore some of those resources in the next section.
Resources for Patients with Thyroid Disease
Support Groups
Many patients with thyroid disease find it helpful to connect with others dealing with similar issues. There are a variety of support groups available for people living with thyroid conditions, both online and in person. Online forums provide an opportunity to ask questions and share experiences without leaving the comfort of home. Local support groups offer face-to-face interaction and can be a great source of information about resources in your area.
Patient Advocacy Organizations
Patient advocacy organizations such as Thyroid UK, The American Thyroid Association, and The British Thyroid Foundation provide valuable information about thyroid health and treatments. These organizations also work to raise awareness about the condition among healthcare professionals, policymakers, and the public at large. They often host events or webinars where patients can learn more about their condition from experts in the field.
Helpful Websites
There are many websites dedicated to providing reliable information on thyroid health topics such as diagnosis, treatment options, lifestyle changes that may help manage symptoms, research updates on new therapies or medications being developed for thyroid diseases, etc. The best website for free information about thyroid and other endocrine diseases is hormone.org (created by the endocrine society).
Contact Information for Local Support Groups
Local support groups can be found through patient advocacy organizations or by searching online directories like Meetup or Facebook Events. Many local hospitals also have listings of nearby support groups on their websites, or you can contact them directly for more information if needed.
FAQs in Relation to Thyroid Disease – a Comprehensive Guide for Patients
What are the new guidelines for thyroid testing?
The American Thyroid Association (ATA) recommends that all adults over the age of 35 should have their thyroid-stimulating hormone (TSH) levels checked at least once every five years. The ATA also suggests that individuals with certain risk factors, such as a family history of thyroid disease or autoimmune disorders, may need to be tested more frequently. Additionally, pregnant women and those taking medications known to affect thyroid function should also receive regular testing.
What are the 3 types of thyroid problems a person can experience?
- Hypothyroidism: This is a condition where the thyroid gland does not produce enough hormones, leading to symptoms such as fatigue, weight gain, constipation and dry skin.
- Hyperthyroidism: This is a condition where the thyroid produces too much of its hormones, resulting in symptoms such as anxiety, rapid heartbeat and weight loss.
- Goiter: Goiter occurs when the thyroid becomes enlarged due to an increase in hormone production or inflammation of the gland itself. Symptoms include difficulty swallowing and breathing, neck swelling and hoarseness of voice.
What is the single most important test to diagnose thyroid function?
The single most important test to diagnose thyroid function is a blood test called the Thyroid Stimulating Hormone (TSH) Test. This test measures the amount of TSH in your bloodstream, which is produced by the pituitary gland and stimulates your thyroid gland to produce hormones. If there are too many or too few hormones being produced, it can indicate an underlying problem with your thyroid. The results of this test will help determine if further testing or treatment is needed for any potential thyroid issues.
Should Thyroid peroxidase antibodies be monitored frequently in Hashimoto’s disease?
The simple answer is no. TPO antibodies are very specific for Hashimoto’s disease and will continue to remain positive for life. As with any autoimmune condition, antibodies can fluctuate over time with or without treatment. Unfortunately, in Hashimoto’s disease the treatment does not involve the use of any medications that alter the level of TPO antibodies. Your antibody levels can change 4 fold in either direction, however the dose of levothyroxine will not change if your TSH (the most important test for hypothyroidism) remains within acceptable limits (defined as the lower half of the normal range)
Why is T3 not checked in hypothyroidism
It is true that free T3 is an active thyroid hormone, and T4 is in effect a prohormone (it is converted to active T3 by the deiodinase enzyme). T3 has a very short half life as such its levels varies quite significantly throughout the day, making random assessment of its level in hypothyroidism very problematic. Furthermore, since TSH levels is produced by the pituitary gland based on the levels of T3 (active hormone), inadequate T3 will inevitably lead to a high TSH. Thus for these reasons, monitoring of T3 is not recommended for either the diagnosis or monitoring of thyroid disease.
Conclusion
Thyroid disease can be a difficult condition to manage, but with the right knowledge and resources, it is possible to live a full life. This comprehensive guide for patients provides an overview of symptoms, diagnosis, treatment options and living with thyroid disease. With this information in hand, you are now better equipped to understand your condition and make informed decisions about your health care.
Remember that thyroid disease is treatable and manageable – don’t hesitate to seek help if you have any questions or concerns about your condition.
The opinions expressed here represent the views of a practicing hormone specialist (endocrinologist) and must not substitute the advice of your health care provider. This blog post is written for a non-medical audience interested in learning more about hormonal disorders. The author has no commercial conflicts of interest to declare. Also, read our privacy policy.
Kindly Let Us Know If This Was helpful? Thank You!

